Hypospadias surgery is the most unrewarding for surgeon and troublesome for the patient in all field on pediatric urology. At the same time it is quite often – 1 in 200 boys has the defect. Such small organ requires 5-40% of reoperation/second stage surgery, depending on primary severity.
The complication may be early and late, local or general, transient and troublesome for years. They affect the anatomy and emotions and sometimes impair the whole family functioning.
Early complications
1. intraoperative bleeding is rather a discomftort for operationg surgeon. Usually can be controlled with bipolar cautery and stasis put at the base of the penis. But it does not like ischemia, which propmotes post operative oedema and impairs healing. So the stasis should be used for shotr periods of time, and coaglation bipolar if any. Postoperative haematoma formation is a common phenomenon, but not desired. It may get infected, but even sterile delays tissue healing. To some extend it may be prevented with subtly compressive dressing. I think every hypospadias surgeon met the situation, when he needed to control prolonged big bleeding again in general anesthesia a few hours after the surgery. Problably this patient have some form of coagulopathy and should be investigated for it.
Sometimes crying or defecation child passes some urine around the catheter and dissolves postoperative clots, making the dressing red. It has nothing to do with bleeding but may worry the parents.
2. Problems with catheter presence and it’s patency. Catheter presence carries great discomfort for the child, increasing with each following day. And also with child’s age and each consecutive surgery. Usually 3 to 7 days is all we can expect from the child. The dyscomfort is intensified during defecation and passing intestinal gas. After a few days a surface of the catheter is infected which caused local irritation and can spread into overt urinary tract infection. The local urethra irritation and infection impair healing. Emotional tolerance of prolonged catheterisation is usually better in first year of life then in toddler. Sometimes is is difficult to maintain catheter patency. The main causes of it’s obstruction is torsion or bending – the parents should actively supervise it. It is absolute basis of hypospadias patient care. Much less often the catheter may get obstructed by debris and clots from the bladder. In this case it should be irrigated. Obstructed catheter makes the child uneasy and finally forces him to urinate around the catheter. The urinae distends the urethra, which ma lead to rupture of freshly sewn sutures and penetration of urine into surrounding tissues. Soaked dressing usually needs to be replaced, which is a stress for a boy.
Palcement on the catheter tip in the bladder is random to some degree and it sometimes drains urine batter, sometimes worse. In this case it is enough that a bady cries or moves rapidly and urine readily passes around the catheter. Sometimes it is simply better to remove such catheter earlier. It is diffictult to judge what promotes fistula formation more- urinating around the catheter or it’s early removal.
The child with indwelling catheter should not be mobile much . Early mobilisation increases the risk of incidental catheter removal, makes it irritate fragile bladder and urethral mucosa, results in bloody urine and pain and iching during following night (don’t know why just in the middle of the night).
Due to emotional factors we usually perform surgery in first year of life, when the child does not have any control over stool. I make additional barriers to protect the penile dressing from it. They cross the perineum and direct the stool backwards. If they have “worked”, they can be easily changed by parents or nurse.Usually the plan is to change the dressing on the 3rd postoperative day. It is multi-layer and tight, so it can be cleaned superficially by parents if slightly contaminated and wait a few hours for complete change.
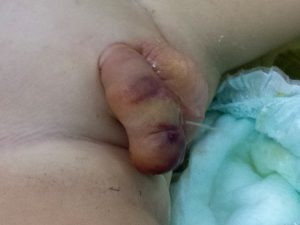
3. Catheter removal is rather simple action, that usually can be done by parents at home. But even here some unusuals situations arise. I remember situation when catheter bent 180degrees inside the bladder and entered the urethra from inside with a diameter doubled in this way. It was neccessary to remove it with force in short general anesthesia. Another time urethral catheter tangled with vesicostomy tube. Somehow the next day they changed position and the urethral one could be removed. Generally it is better not to place too much catheter inside. Baloon Foley catheters are known to malfuntion from time to time – the ballon cannot be deflated and the catheted in anchored in the bladder.
First voiding after catheter removal may be accompanied by some pain or discomfort – it is normal. From the other hand it is critical moment, especially when long parst of urethra had been reconstructed. It tends to be rigid and uncompliant, sometimed narrow in most distal glanular part (operatin g surgeon should remember and prevent it). It may act as an obstacle for the urine, which searches for the shorter way. It can penetrate between the sewing line, get under the skin and form cutanous fistula. Everything may get swollen and finally effective passage of urine is impossible. The only solution is placing a catheter through the urethra (which is rarely possible) or puncture vesicostomy in short general anesthesia. Usually after a couple of weeks penis and urethra heal nad micturition is possible. Vesicostomy tube may be removed, the puncture wound heals sponataneously. The final repair of the fistula that usually remains is delayed for at least 6 months. Sometimes the oedema of the penis, that formed in this circumstances persists for months.
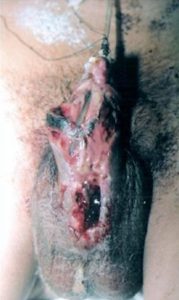
4. Wound infection. Every surgical wound may get infected. Sterilisation of surgical equipment, aseptical enviroment of operating facility, antibitic prophylaxis, carful surgical technique that limits haematoma formation and skin ischemia all may lower the frequency of wound infection butcannot eliminate it completly. Every skin, and specially skin of glans, penis and perineum in a neonate are colonized by typical skin and fecal bacteria which easily infect the wound. Every hypospadiologist knows the feeling of helplessness and disappointment when observing flourishing infection and penis wound separation, after he smartly reconstructed everything making wide urethra, reconstructed corpus spongiosum, penis was big and manageable. During the catheter period wound care constists of regular daily dressing change (not welcome by the patient) and local antibiotics (bacitracin). Sometimes it is wise to change prophylactic general
Penile wound infection and dehiscence
antibiotic for a broad spectrum one, especially when fulminant skin necrosis is observed. After removal of the catheter things get easier -water, local antibiotic and sterile compresses are applied by parents. The wound may look different depending on particular bacteria species. Sometimes it is stinging yellow/grees pus, sometimes mucus, otherwise it is just reddening and wound separation through all planes of surgical preparation. Rarely infection leads to fulminant skin necrosis – brown/black hard scab, that can mimic haematoma at very beginning. General broad spectrum antibiotic sometimes helps in spectacular manner. There is no place for bacterial culture, or at least it has no practical role. The antibiotic is a choice of the surgeon.

5. Skin necrosis. Generally penile skin is supplied with blood vessels reletively well. It allows creating skin flaps, mobilisation of them, it even accepts degloving. Sometimes we observe symptoms of partian skin ischemia secondary to oedema and haematoma. Collections of fluid form under epidermis, resembling sunburns. They evacuate spontaneously with no consequences. Techniques utilizing “neighbouring” skin with no fancy flaps rarely lead to real full thickness necrosis, and probably the cases that happen have something to do with wound infection. From the other hand soft and thin mobilised skin of the penis may have much lesser potential for healing and here every stich matters.
6. Hematuria. Pink or reddish urine is normal when a catheter is placed in the bladder. It’s lining is fragile and prone to some superficial bleedeing. The phenomenon is intensified, when a child is allowed to play and move a lot. Somehow daily activity intensified catheter dyscomfot in the night. Generally it is better to immobilise a child as much as possible. Hematuria has different aspect in children in whom we create temporary vesicostomy. The needle used for vesicostomy creation is quite thick and it’s tip may cut muscules or bladder wall vessels leading to quite intense bleeding, resulting in cherry-like coloration of urine. Usually it is transient, but if lasts for 2 or 3 days we must check hematocrit – I remebmer boys that required blood transfusion. This patients should stay in hospital unti the situation is clarified.
7. Emotional aspects, sexual identity etc. The penis is very special organ for boys big and small. All trauma in this region hurts much. The only exception is neonatal age – the penis is less important and behid vision and reach. Mother presence and basic needs are what counts most. Taht’s why most pediatric urologists tend to perform hypospadias correction in late neonatal age. Behind 18 months of age all manipulation in this area, especially painfull, and indwelling catheter cause great fear and torment. Often these boys don’t sleep in the nightm when catheter is somehow most disturbing. They violently protest agains any medical actions. Sometimes hypospadias repair makes a chid step backward as far as voiding control is concerned. They return to diapers for some time – parents are anxious about it. That’s why we should try to limit a number of dressing changes and not prolong the “catheter period” to much. It is better to create vesico-cutaneous shunt then torture the child with urethrac catheter. It is welcome if the parent actively engage in basic care – care of catheter patency and prevention of stool contamination. Every approach of a nurse is stressful for little patient. I’ve known patients in whom multi-stage treatment had detrimental impact on whole family function. Correcting hypospadias in older age leaves the patients with uncomfortable awareness of being “hypospadias man”. Unfortunately pediatric urologist rarely has an opportunity to meet these patients in adulthood and learn how thy are doing.
8. Parents – one can wonder why in “complications” chapter. Anesthesia and surgical procedure are big stress for the parents. Also the postoperative period, at least days with a catheter, is a test for their patience and determination. And final effect is uncertain and clear after 2 months. The way the parents deal with all this has great importance for child’s comfort and relation with surgeon. I’ve met very composed people facing real complications and ones that party the evening after the surgery. They come smelling the next day with catheter that is twisted 20 times….9
9. Urinary tract infection. Introduction and prolonged presence of the catheter in the bladder increases rosk of urinary tract infection. The probability of this is directly proportional to lenght of “catheter period” or in patients with 3 weeks vesico-cutaneous shunt. Antibiotic prophylaxis is obligatory – regular antibiotic (like cefuroxime), sulfametoxazole+trimetoprin or at least nitrofurantoine. I remember a few patients who developed resistant infections, which required intravenous therapy with more sophisticated drugs in pediatric ward. Well known pathogen of reconstructe urethrae is Pseudomonas aeruginosa which likes skin-made urethra or hair in the urethra of older patients. It’s presence sometimes is symptom-free and can be named colonisation, not infection.
All above mentioned factors can appear together and in combinations.
All this makes it better to perform surgery close to place of residence, especially when going home with catheter in the urethra. This whole periord plus a few days after catheter removal the patient should have easy access to pediatric urologist, preferably the one who performed the procedure. From the other hand staying with catheter in hospital does not guarantee safety. Once I’d got the call from desperate mother who stayed with her son in hospital – he was suffering and voiding aroung he catheter. The doctor on duty (pediatric surgeon) ordered morphine (which is never neccessary after penile surgery) by phone. In the morning it turned out the cathter was twisted. It would suffice to just check it, and maybe flush with saline…
In my opinion the best partner in hypospadias child care are engaged, educated and calm parents, who take care about the dressing and catheter themselfes as much as possible, according to instructions.
Late complications
1. Urethral fistulas – are the most common and troublesome complication of hypospadias. Urine is flowing from the tip of the penis (our new orifice) and simultaneously by one or more openings in the shaft of penis, which are unwanted ones. It usually forces a chile to urinate in sitting position. The longer the urethra we create the greater the probability of fistula formation, because urine “looks for” shorter way out. The next correcting procedure can be performed not earlier then 6 months after the first one. Common location of the fistula is retroglanular region, covered be prepuce. The tissues here are thin and poorely vascularised. Usually the fistura here cannot be just closed – recreation of whole glanular urethrae is neccessary. From the other hand a small needle-like fistula here, which yields only single drops of urine, is accepted by patients as minor hygienic incovenience and they refuse surgery. Fistula on shaft of the penis is greater problem – urine drops on shoes and forces the patient to urinate in sitting position. We should tend to close those in infancy because of psychological reasons. Small fistula on the shaft requires a catheter just for 3 days, whereas longer defect will not heal without cystostomy creation.
2. Urethral stricture formation- is I think the most troublesome remote hypospadias complication, and to some degree it’s likeliness depends on surgeon’s skills and intraoperative decisions. Though sometime s reall wide-created urethra can narrow. Some strictures, especially those of urethral meatus, are prone to be cured just with a few calibrations, in local anesthesia. From the other hand long strictures can be asymptomatic for long time because bladder muscle compensates and overgrows. Then it fails, cannot empty competly, urinary infection often ensues. Partial urinary incontinence or dibbling is also possible. Sometimes even the upper urinary tract dilates. Surgical treatment of strictures is troublesome (especially in small children), is not easy and has it’s own complications. The best results are achived when a patient is convinced to do himself or accept daily dilation/calibration of the urethra at home.
3. Urethral diverticula are usually secondary go urethral stricture and develop proximally to it, where the urethra dilates. During urination we can see a ball-like or pelican neck-like swelling in proximal penile or scrotal region. Then for a couple of minutes the urine gradually evacuates from the diverticulum and makes the underwear wet or forces the patient to patiently milk it out. Often untreated diverticulum will grow with time. Dilation of stricture or rarely it’s incision will allow the diverticulum to shrink with time. Though I remember boys in whom surgical reduction of urethral excess was neccessay.

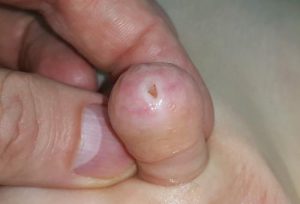
4. Phimosis. It can always happen after the hypospadias surgery. Trying to reach good cosmetic result we sometimes make it too narrow, otherwise typical aquired BXO phimosis may develop (picture on the left). Often I correct the phimosis during primary hypospadias surgery incising it on dorsal side. Later correction usually is simple, does not require catheterisation but general anesthesia is neccessary.
5. Difficult catheterisation of reconstructed urethra. Catheterisation may be difficult due to various reasons, independant of prior hypospadias surgery. Reconstructed urethra may have uneven shape, may have small diverticula, kinks and so on. On occasion unaware and untrained doctor or nurse will have problem with it. The patient should always inform about his condition if possible. Catheterisation should be gentle and careful to find the right way. Curved Tiemann catheter is very useful in this situations.
7. Circumcised look. In most cases of hypospadias the fore skin can be easily reconstructed. This is also the the wish of most patients in our country. Some techniques of hypospadias reconstruction utilize preputial skin for reconstruction of the urethrae. In my opinion this makes sense only in complicated redo cases. Unfortulately some doctors copy methods from anglo-saxon professional books one-to-one, with no thought of their own, not even informing patients that the foreskin will be sacrificed. Removed of used foreskin can not be reconstructed.
8. “Fistula” or additional openning in the foreskin. Reconstruction of the foreskin may end up with partial wound dehiscence and creation of additional, usually small, openning. This is just cosmethic defect, no urine is passed through this openning. Surgical correction is not a great discomfort, no catheter in the urethrae is neccessary.
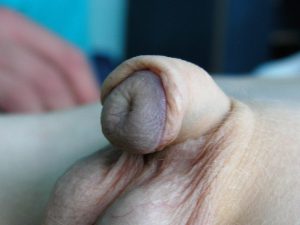
9. Penile curvature and other permanent deformations. Sometimes the deformation is residual, slightly expressed and not impairing sexual function. Also residual rotation is acceptable – it is very hard to correct it. But unfortunately sometimes it is a result of unwise surgeons decision, as the penis on the left. Widely accepted technique of correction of primary retroglanular hypospadias is Snodgrass TIP (surrounding skin is used to create short lacking urethra)In this patient the uretha was totally mobilised (and devascularised) just to pull it the 3-5mm. I was also fixed a bit on the back of the glans. Because it was devascularised it behaved as free graft and contracted significantly. The result is curved, ugly penis with flattened glans. This is extremly difficult to corect it.